|
Postoperative delirium (POD) is a life-threatening condition recognized by the American Geriatric Society as a prevalent postoperative complication. Considering the high occurrence of MCI in the elderly, it is intriguing to explore its possible connection with adverse postoperative results. However, this rate can soar to 87% among nursing home residents. In the broader community, MCI is frequently diagnosed among elderly individuals, with an incidence rate of approximately 17%. Frailty has been linked to an increased risk of memory function deficits, including mild cognitive impairment (MCI) and dementia. Frailty, a state of accumulated physiological deterioration across various organ systems in elderly individuals, has been reported to be a better predictor of perioperative adverse events than age alone. It has been documented that 53% of all surgical procedures are performed in this population segment. Īs longevity may correlate with a rise in morbidities over time, conditions requiring medical or surgical intervention are major concerns for elderly individuals. This proportion is expected to surge to 28% within the next decade. 
Of Thailand’s 67 million inhabitants, 12 million (17.9%) are considered elderly. Thailand stands out as one of the Asian nations with the most accelerated aging rate. Approximately 60% of all individuals aged 60 years and above reside in Asia and the Pacific region. 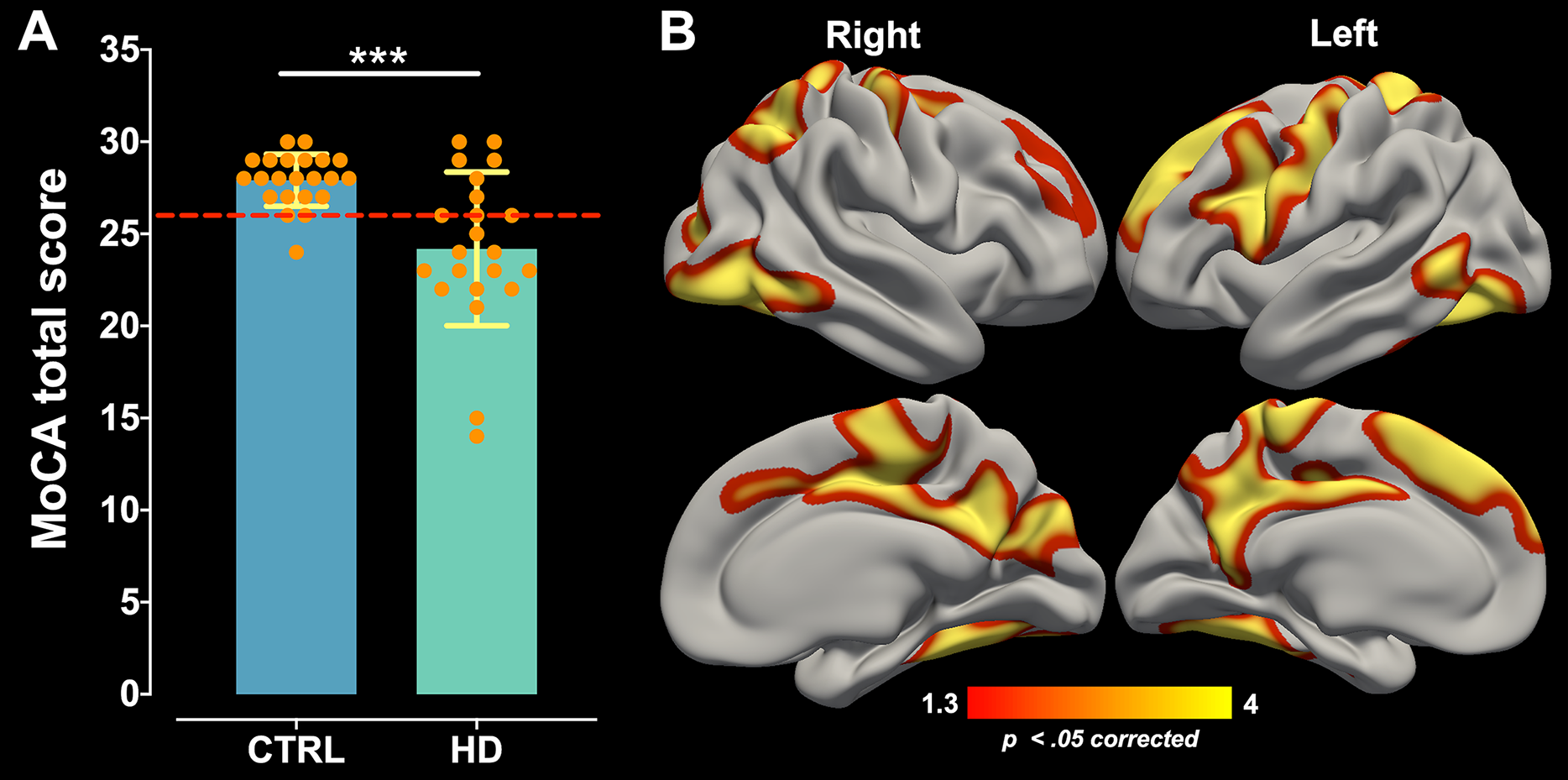
This proportion is projected to climb to 26% by 2050. The number of individuals aged 60 and older has increased exponentially, reaching 670 million in 2022 and accounting for 14% of the world’s population. With socioeconomic development and medical advancements, the global population is rapidly increasing. This trial was retrospectively registered in the Thai Clinical Trials Registry on (registration number: TCTR20190115001). These findings underscore the importance of postoperative cognitive assessments for both elderly patients with preexisting MCI and those with previously intact cognitive functions. This was identified by a reduction in postoperative MoCA scores for the visuospatial, naming, attention, language, abstraction, and orientation domains. However, the non-MCI group demonstrated a higher incidence of POCD than the MCI group. 
The incidence of POD was similar in the MCI and non-MCI groups. Postoperatively, the MCI group notably declined in visuospatial, attention, and orientation domains, while the non-MCI group declined in all domains except delayed recall. There were no significant differences in other postoperative complications between the groups. POCD occurred in 24.3% of MCI patients and 50% of non-MCI patients ( P = 0.001). The incidence of POD was 16.6% in the MCI group and 14.3% in the non-MCI group ( P = 0.839). The study comprised 223 elderly patients with MCI and 56 without MCI. Secondary outcomes encompassed other postoperative complications, including POCD. The primary outcome was the incidence of POD within the first 72 h postoperatively. POCD was characterized by a MoCA score reduction of 2 or more points from the preoperative score. POD was diagnosed using criteria from the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5). Preoperative MCI was determined by a Montreal Cognitive Assessment (MoCA) score between 18 and 24. MethodsĪ prospective study enrolled patients aged 60 years and above scheduled for major surgeries between December 2017 and April 2022. 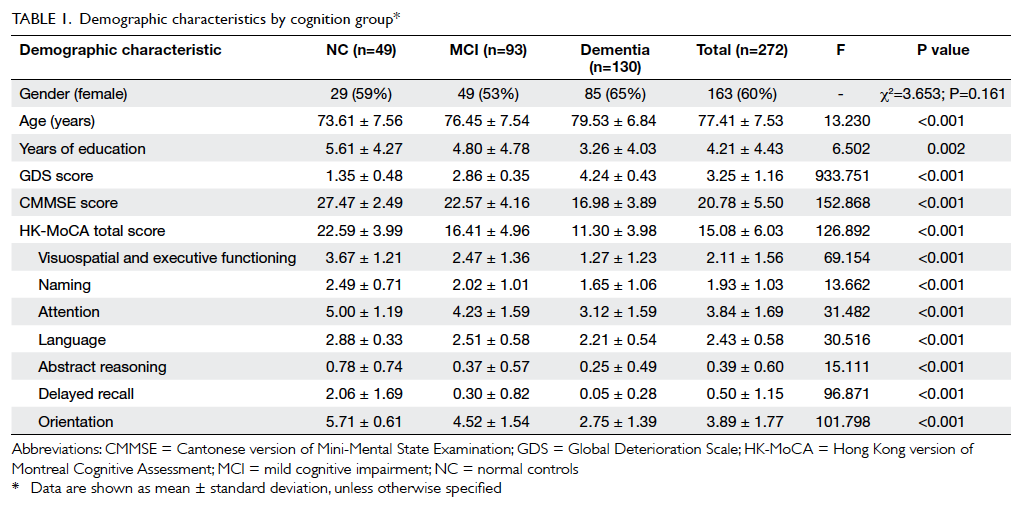
This study aimed to determine the incidence of POD in elderly patients with and without preexisting MCI. However, the correlation between MCI and POD remains unclear. Most of these patients already have preoperative mild cognitive impairment (MCI). Postoperative delirium (POD) and postoperative cognitive dysfunction (POCD) frequently occur in older surgical patients. As societies age, increasing numbers of older adults undergo surgeries with anesthesia.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
